September 20, 2022
by Carla Hay
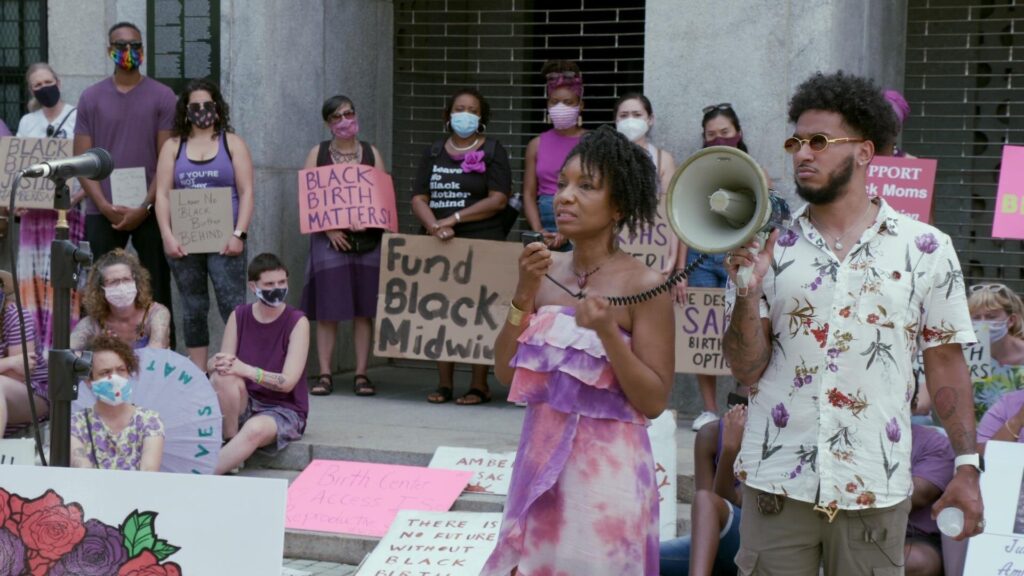
Directed by Paula Eiselt and Tonya Lewis Lee
Culture Representation: Taking place in New York City, Boston, Houston and Tulsa, Oklahoma, the documentary film “Aftershock,” which was filmed from 2019 to 2021, features a predominantly African American group of people (with some white people and a few Asians) talking about the systemic racism in U.S. maternal health care that results in a disproportinately high death rate of African American women who died from childbirth or complications from childbirth.
Culture Clash: Family members of African American women who died in hospitals during childbirth have become activists to try to end systemic racism in maternal health care, but they face uphill battles and resistance from people who want to enable or deny this racism.
Culture Audience: “Aftershock” will appeal mainly to people who are interested seeing true stories about how race relations and social classes affect the type of health care that people get in the United States.

“Aftershock” is a disturbing but necessary documentary to watch for a reality check about how systemic racism in the U.S. health care system has resulted in black women dying after childbirth at disproportionately higher rates than other races. The film isn’t just about spouting statistics and facts, although that important information is included. What will emotionally resonate with viewers the most are the stories of real people whose lives have been permanently changed by these medical injustices.
Directed by Paula Eiselt and Tonya Lewis Lee, “Aftershock” is a no-frills documentary that thankfully isn’t overstuffed with too many talking heads. “Aftershock” (which is Lewis Lee’s feature-film directorial debut) had its world premiere at the 2022 Sundance Film Festival, where “Aftershock” won the U.S. Documentary Special Jury Award called Impact for Change. “Aftershock,” which is filmed and edited clearly and concisely, is certainly the type of documentary that will motivate people to want improvements in the U.S. medical care system.
“Aftershock” essentially tells three main stories of African American people who’ve been affected by maternity health care in the United States. Two of the stories are about two families coping with the deaths of a woman in their family who died after childbirth. The third story is about a married couple who have to decide if the pregnant wife will give birth in a hospital or opt for an alternative location. Meanwhile, some experts and activists weigh in with their perspectives and sharing of information.
One of the documentary’s main stories is about the aftermath of the October 2019 death of 30-year-old Shamony Gibson, who died in New York City from pulmonary embolism (blood clotting in the lungs), 13 days after giving birth by C-section to her second child, a son named Khari. “Aftershock” shows how Gibson’s mother Shawnee Benton Gibson and Gibson’s partner Omari Maynard (the father of Khari) became activists as a result of Gibson’s death, which they believe could have been prevented if she received adequate medical care from the medical professionals who knew about her blood clot symptoms.
Before she died, Gibson had been suffering from shortness of breath and chest pains, which are two symptoms of pulmonary embolism. Gibson’s reported these health problems to medical professionals, who dismissed her concerns and told her that she just needed to rest more. According to Gibson’s family, she also was repeatedly asked by medical professionals, “Are you on drugs?”
Gibson was not using drugs, and the medical people were repeatedly told that information, but they didn’t seem to believe it, because they kept asking the same question. The family members believe that the medical people who repeatedly asked this “Are you on drugs?” question would not have been so stubborn in assuming that Gibson was a drug user if Gibson were a white person. They also believe that medical professionals would not have been so quick to dismiss Gibson’s health problems if she were white.
Unfortunately, the hospital where Gibson was taken was underfunded and understaffed. According to Gibson’s family (including her sister Jasmine Gibson, who is interviewed in “Aftershock”), Gibson was taken to the emergency room, where she had to wait 12 hours before getting medical treatment. By then, it was too late. She died at the hospital.
In “Aftershock,” Benton Gibson says that she worked at the hospital as a loyal employee for 25 years and never thought that the hospital would play a role in her daughter’s death. It was a rude and tragic awakening that fuels a lot of Benton Gibson’s activism. One of her biggest messages, particularly to Black women who give birth, is to not be fooled into thinking that what happed to her daughter can’t happen to them.
Another documentary story is about what happened after the April 2020 death of 26-year-old Amber Rose Isaac, who passed away after having a C-section at Montefiore Hospital in New York City’s Bronx borough. Isaac’s son, Elias Isaac McIntyre, survived the C-section, but Isaac did not. Bruce McIntyre (Elias’ father) eventually met Maynard, and they formed a support group for single fathers whose partners died from maternity health care that’s believed to be inadequate and rooted in racism.
While in the hospital for the childbirth, Isaac was diagnosed with HELLP (Hemolysis, Elevated Liver enzymes and Low Platelets) syndrome, a pregnancy complication that affects the blood and liver. Isaac’s family members believe medical negligence caused Isaac’s death and are suing Montefiore Hospital with this claim. The plaintiffs’ lawsuit contends that Isaac could have been diagnosed with HELLP syndrome long before she was in the hospital to give birth. Isaac’s family also believes that Isaac would have received better medical attention if she were white.
The third main story in “Aftershock” follows married couple Felicia Ellis and Paul Ellis as they prepare for the birth of their first child in Tulsa, Oklahoma. Felicia and Paul know about the horror stories about black women (especially low-income black women) getting treated as inferior in the U.S. health care system, compared to women of other races. The documentary shows Felicia and Paul being wary of Felicia going to a hospital for the birth of their child and looking into the birth center Breathe Birth and Wellness as an alternative. The documentary includes footage of Felicia giving birth.
It would be very easy for skeptics to say that people are just being paranoid when it’s pointed out that racism exists in the U.S. health care system. However, plenty of statistics from independent reports back up the racism claims. “Aftershock” has those statistics, which are also publicly available to anyone who wants to find them.
One of the alarming trends is that childbearing black women in the U.S. are more likely than childbearing women of other races to be told that they need a C-section when giving birth. C-sections take less time than vaginal births, but because C-sections are surgeries, women giving birth are more likely to die fom C-sections than from vaginal births. In addition, “Aftershock” points out the cold, hard fact that hospitals get more money from C-sections than they do from vaginal births.
Helena Grant, director of Midwifery at Woodhull Medical Center (a public health facility in New York City), comments in the documentary: “Very early on in my career, black women were used as guinea pigs.” Grant, who is also a certified nurse-midwife (CNM), mentions that people training in obstetrics and gynecology (OB-GYN) in the U.S. usually do their training in hospitals and clinics in low-income communities, which are often largely populated by people of color. These inexperienced OB-GYN professionals are more likely to be the lowest-paid in the OB-GYN field and most likely to make mistakes. And guess who suffers the most as a result?
Multiple people in the documentary mention that Black women are at the most risk of getting the worst maternity health care in the U.S. because of attitudes that still linger from the enslavement of black people in America. Enslaved black women were considered “property,” not human beings, and therefore were not given the health care that people who were not enslaved were entitled to get. There’s also a persistent misconception, stemming from America’s shameful slavery history, that black women are more tolerant of physical pain than women of other races.
“Aftershock” also mentions how patriarchal and sexist attitudes changed practices of assisting during childbirth. Before the 20th century, midwives and home births used to be more common in the U.S. than they are now. During the years when slavery was legal in the U.S., enslaved black women were often the midwives for the white families who enslaved them.
When men wanted to take over the practice of assisting during childbirth and make money from it, the OB-GYN profession was born in the 1700s. In the OB-GYN profession’s earliest years in the U.S., the profession was open only to people who had access to a getting a medical degree, which usually meant white men only. And although medical schools in the U.S. can now enroll people of all races and genders, to this day, most OB-GYN doctors in the U.S. are white men.
“Aftershock” also mentions the money-motivated campaign that began the early 1900s to get more women to go to hospitals to give birth, in order to take business away from midwives who helped women give birth in places other than hospitals. There are certainly advantages to having a doctor rather than a midwife assist in childbirth. However, “Aftershock” shows that more people are considering alternatives to giving birth in a hospital (options include licensed birth centers or home births) if they think the hospital will be giving incompetent care due to a patient’s race.
Neel Shah, professor of obstetrics and gynecology at Harvard Medical School, comments: “I think the well-being of moms is the bellwether for the well-being of society in general. That’s why every injustice in society shows up in maternal health care.” Shah also notes that it wasn’t until 2018 that the U.S. federal government began tracking maternal health trends. Many racial disparities can be found in these trend reports.
“Aftershock” includes footage of Shah leading an OB-GYN seminar, with McIntyre as a guest speaker. The seminar’s students (who are mostly women of various races) are visibily moved by McIntyre’s story and seem to have learned a lot from his personal account of how racism can affect the health care that someone can get. One of the students speaks to McIntyre after his talk and says to him that she had heard about Isaac’s death on Twitter, but it made a difference to see firsthand how her death affected someone in Isaac’s family.
“Aftershock” also has powerful moments of Benton Gibson, Maynard and McIntyre doing activism work to try to raise awareness about racism in maternity health care and to pass better laws about maternity health care. They attend rallies and do community outreach in these endeavors. In one scene, Benton Gibson passionately testifies during a New York City Council hearing on maternal health. New York City Council member Carolina Rivera expresses her support of Benton Gibson during this hearing.
In New York City’s Brooklyn borough, Maynard and McIntyre choose Weeksville Heritage Center as a meeting place for other single fathers who have experienced similar tragic losses of their partners who died from childbirth-related deaths. Maynard says of this meeting place: “I want to create a space where we can star to try to change policy, where we can have hundreds of thousands of people backing what we’re saying, because that’s the only way it works.”
Maynard, who is an artist who paints portraits, also began painting portraits of other women of color who died as a result of inadequate maternity health care. Maynard has met many of these women’s families through his advocacy/activist work, and he gives these portraits as gifts to the surviving family members. In one of the documentary’s emotionally potent scenes, Maynard gives a portrait of the late Maria Corona to her surviving partner Sam Volrie Jr., who is moved to tears by this gift.
Other people featured in the documentary include registered nurse Giselle Chebny; certfied nurse-midwife Regina Kizer; and Tulsa Birth Equity Initiative executive director LaBrisa Williams; and doulas Nubia Martin, Ashlee Wilson and Myla Flores. Toward the end of the documentary, Maynard and McIntyre are shown making plans to eventually open birth center in the Bronx, with the intention to help low-income pregnant women in particular, since these low-income women are less likely to get the proper medical care that they need.
“Aftershock” is not propaganda for birthing centers, nor is it a sweeping and unfair condemnation of all hospitals and OB-GYN medical professionals. However, the documentary does a very good job at sounding the alarm that pregnant black women in America are more likely to die from inadequate or incompetent medical care than pregnant women of other races. “Aftershock” is an effective presentation of facts and human stories to serve as a reminder that this problem is not just a concern for people of color but for all people who are against racism.
Hulu premiered “Aftershock” and released the movie in select U.S. cinemas on July 19, 2022.
